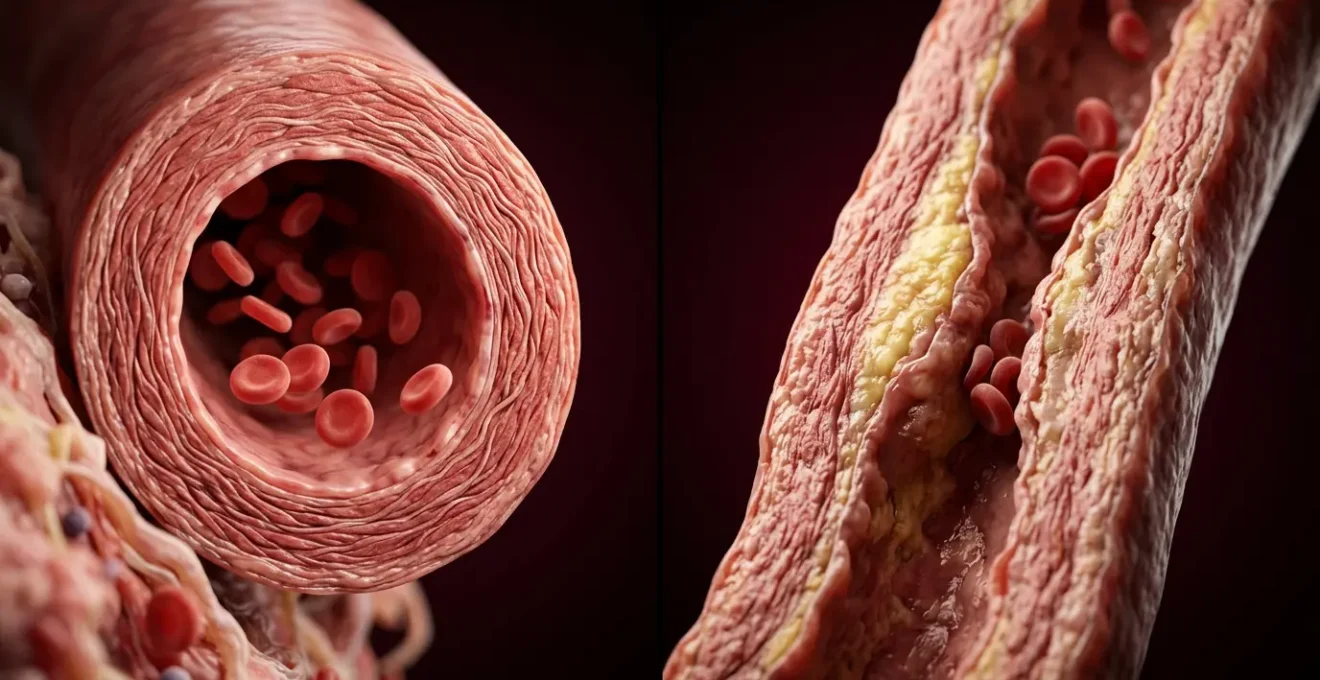
Contrary to common belief, early arterial stiffening isn’t just about high cholesterol or blood pressure; it’s driven by hidden metabolic saboteurs that silently damage your arteries from the inside out.
- High blood sugar acts like ‘sandpaper’ on your arterial lining, initiating damage years before a high glucose reading appears on a test.
- Key nutrients like Vitamin K2 and natural compounds in foods like beetroot play a critical role in maintaining arterial flexibility, a factor often overlooked.
Recommendation: Shift your focus from traditional markers alone to understanding and managing your metabolic health—specifically fasting insulin and inflammation—to truly protect your vascular future.
It’s a disconcerting feeling for many in their 30s and 40s: a sense that your body is aging faster than it should. You follow the standard advice—you watch your cholesterol, you try to manage stress, and you get your blood pressure checked. Yet, a silent process may be underway, making your arteries, the vital highways for your blood, become stiff and brittle, a hallmark of aging that seems to be accelerating in younger generations. This isn’t just a feeling; it’s a physiological reality for many dealing with the pressures of modern life, high-stress jobs, and diets of convenience.
The conventional wisdom points to smoking, high blood pressure, and high LDL cholesterol as the primary villains of vascular health. While these are undeniably critical factors, they don’t tell the whole story, especially when it comes to this premature hardening. The conversation often stops just when it should be getting deeper. What if the real damage starts much earlier, at a microscopic level, driven by factors your annual physical might not even be screening for? What if the key to protecting your arteries lies not in simply managing numbers, but in understanding the underlying metabolic chaos that causes them to rise in the first place?
This guide moves beyond the surface-level advice. We will uncover the hidden mechanisms that act as the true architects of early arterial stiffening. Instead of repeating platitudes, we will explore the ‘why’ behind the damage: why high blood sugar erodes your arteries, how specific nutrients and exercises can restore flexibility, and why metrics like fasting insulin are far more predictive of your future health than the cholesterol number you’ve been taught to fear. This is a new framework for thinking about vascular longevity, giving you the power to intervene before the damage becomes irreversible.
To navigate this crucial topic, we will explore the specific mechanisms and actionable strategies that can make a difference. This article breaks down the science into manageable parts, providing a clear roadmap to understanding and improving your arterial health.
Summary: Why Are Your Arteries Stiffening Earlier Than Your Parents’ Did?
- Why Does High Blood Sugar Act Like ‘Sandpaper’ Inside Your Arteries?
- How to Use Beetroot Juice to Relax Your Arteries Naturally?
- Vitamin K2 or Calcium: Which Actually Keeps Plaque Out of Your Arteries?
- The ‘Silent Killer’ Mistake That Damages Kidneys Before You Feel It
- How to Use Stretching and Yoga to influence Arterial Stiffness?
- Why High Fasting Insulin Is a Red Flag Your GP Might Not Mention?
- Why Does Slow Jogging Build More Energy Factories in Your Cells Than Sprinting?
- Why Is Cholesterol Not the Only Number That Matters for Your Heart?
Why Does High Blood Sugar Act Like ‘Sandpaper’ Inside Your Arteries?
The damage from high blood sugar begins long before a diagnosis of diabetes. Think of the inner lining of your arteries, the endothelium, as being coated with a delicate, non-stick gel layer called the glycocalyx. This microscopic barrier is your first line of defense, repelling plaque and blood cells to ensure smooth, unimpeded blood flow. However, chronically elevated blood sugar acts like abrasive sandpaper on this fragile layer, physically eroding it. This erosion compromises the barrier’s integrity, making it more permeable.
Once the glycocalyx is damaged, the underlying endothelial cells are exposed. This triggers a cascade of inflammatory responses. Furthermore, excess sugar in the blood leads to a process called glycation, where sugar molecules attach to proteins and fats, creating harmful compounds known as Advanced Glycation End-products (AGEs). These AGEs are particularly destructive; they cause the collagen and elastin fibers within the arterial walls to become cross-linked, stiff, and less flexible. This process is not abstract; research from the American Journal of Physiology demonstrates a significant increase in the passage of harmful substances across the endothelial layer under high-glucose conditions, confirming this “leaky” and damaged state.
This progressive damage is why metabolic health is so critical. The stiffening isn’t a sudden event but a slow, gradual degradation initiated by metabolic dysfunction. The constant “sanding” effect from high glucose sets the stage for atherosclerosis, where cholesterol and other substances can more easily adhere to the damaged arterial wall, forming the plaque that leads to serious cardiovascular events. It’s a silent process that underscores the importance of managing blood sugar levels well before they reach a pre-diabetic or diabetic threshold.
How to Use Beetroot Juice to Relax Your Arteries Naturally?
One of the most effective natural strategies for combating arterial stiffness involves harnessing the power of nitric oxide (NO), a potent vasodilator that signals your arteries to relax and widen. Stiff arteries are often characterized by endothelial dysfunction, a condition where the inner lining of the arteries loses its ability to produce adequate amounts of NO. This is where beetroot juice emerges as a powerful therapeutic tool. Beetroots are exceptionally rich in inorganic nitrates, which your body converts into nitric oxide.
When you consume beetroot juice, the nitrates are quickly absorbed into your bloodstream. Salivary glands play a crucial role, converting these nitrates into nitrites. Once in the acidic environment of the stomach, or through the action of various enzymes in your tissues, these nitrites are then converted into nitric oxide. This boost in NO availability has a direct, measurable effect on your blood vessels, improving their elasticity and ability to dilate, which in turn lowers blood pressure and reduces the strain on your heart.
The impact is not just theoretical; it’s clinically proven. A single dose of beetroot juice can significantly improve vascular function. For instance, a clinical trial found a 0.59 m/s reduction in arterial stiffness, measured by pulse wave velocity, in subjects who consumed nitrate-rich beetroot juice. This demonstrates a direct and relatively rapid improvement in arterial flexibility. Incorporating beetroot juice into your diet, whether as a daily shot or mixed into smoothies, offers a practical, food-based method to support your body’s natural mechanism for maintaining supple, healthy arteries. It’s a direct intervention to counteract the stiffening process.
Vitamin K2 or Calcium: Which Actually Keeps Plaque Out of Your Arteries?
The conversation around arterial plaque often focuses on calcium, but this misses the crucial half of the equation. The problem isn’t calcium itself, but where it ends up. This is known as the “calcium paradox”: our bodies need calcium for strong bones, yet its deposition in soft tissues like arteries leads to calcification and stiffness. The key to solving this paradox lies not in avoiding calcium, but in properly directing it. This is the specialized job of Vitamin K2.
Vitamin K2 acts as a traffic cop for calcium in the body. It activates two critical proteins: osteocalcin and Matrix Gla Protein (MGP).
- Osteocalcin, once activated by K2, helps bind calcium to the bone matrix, strengthening your skeleton.
- Matrix Gla Protein (MGP) is the most potent inhibitor of soft tissue calcification known. When activated by K2, MGP actively patrols your arteries, binding to free-floating calcium and preventing it from depositing in the arterial walls.
Without sufficient Vitamin K2, these proteins remain inactive. Calcium is not effectively directed to the bones and is free to accumulate in the arteries, leading to vascular calcification—a primary driver of arterial stiffness.
To put this in perspective, think of the difference between strong bone and a brittle, calcified artery. One is a sign of health, the other a sign of disease, yet both involve the same mineral. The differentiating factor is the presence of an intelligent guidance system provided by Vitamin K2.
As this visual contrast suggests, ensuring adequate K2 intake is fundamental for long-term cardiovascular health. While calcium supplements have been controversially linked to increased cardiovascular risk, this is often in the context of K2 deficiency. Sources of Vitamin K2 include fermented foods like natto, hard cheeses, and grass-fed animal products. Ensuring its presence is a non-negotiable strategy to keep your arteries flexible and your bones strong.
The ‘Silent Killer’ Mistake That Damages Kidneys Before You Feel It
Arterial stiffness is often called a “silent killer” because its most severe consequences can develop without any noticeable symptoms until significant damage has occurred. One of the most common and dangerous mistakes is underestimating the profound impact of stiff arteries on your kidneys. Your kidneys are a dense network of tiny, delicate blood vessels (glomeruli) responsible for filtering waste from your blood. Their health is directly dependent on receiving blood flow at a stable, controlled pressure.
Healthy, elastic arteries act as a buffer, absorbing the pressure wave generated by each heartbeat and smoothing it out to deliver a gentle, continuous flow to the organs. Stiff, rigid arteries lose this buffering capacity. Instead, the full, pulsatile force of each heartbeat is transmitted directly to the delicate kidney filters. As a vascular health specialist, I often use a specific analogy to explain this to patients. As Raymond Townsend, M.D., of the University of Pennsylvania School of Medicine, aptly describes:
The high ‘pulse pressure’ from stiff, non-compliant arteries acts like a physical jackhammer on the delicate filtering units of the kidneys.
– Raymond Townsend, M.D., University of Pennsylvania School of Medicine
This relentless “jackhammer” effect physically damages the glomeruli over time, leading to chronic kidney disease. The process is insidious; you won’t feel it happening. Your kidney function can decline significantly before any symptoms like fatigue or swelling appear. This connection is not minor; the Framingham Heart Study demonstrated a 48% increased likelihood of developing cardiovascular disease with increased arterial stiffness, a risk that is tightly linked with declining kidney health. Ignoring arterial stiffness is therefore a critical mistake that puts the long-term function of these vital organs at severe risk.
How to Use Stretching and Yoga to influence Arterial Stiffness?
While aerobic exercise is well-known for its cardiovascular benefits, the influence of practices like stretching and yoga on arterial stiffness is an equally important, though less discussed, aspect of vascular health. The mechanisms are multifaceted, involving both direct physical effects and systemic benefits. Chronic tension in major muscle groups, particularly in the trunk and legs, can physically compress the large arteries that run through them, contributing to increased stiffness and resistance to blood flow.
Regular, deep stretching helps to release this muscular tension, directly reducing the external pressure on the arteries. Furthermore, practices like yoga incorporate controlled breathing (pranayama) and mindfulness, which have a profound effect on the autonomic nervous system. By shifting the balance away from the “fight-or-flight” sympathetic response towards the “rest-and-digest” parasympathetic response, yoga helps lower systemic inflammation, reduce stress hormones like cortisol, and increase the production of nitric oxide—all of which promote arterial relaxation and flexibility.
The benefits are supported by a growing body of evidence. Studies show that practices like yoga and Tai Chi consistently improve measures of arterial stiffness, such as pulse wave velocity (PWV). These benefits are particularly pronounced in individuals with hypertension or obesity, indicating that these modalities can be powerful therapeutic interventions. Even a single session of aerobic exercise can result in lowered arterial stiffness for a period of 30 minutes to 24 hours afterward. Integrating consistent stretching or a regular yoga practice complements traditional cardio by addressing the interconnected roles of muscular tension, stress, and nervous system regulation in maintaining vascular health.
Why High Fasting Insulin Is a Red Flag Your GP Might Not Mention?
In a standard physical, the focus is often on fasting glucose. If that number is normal, you’re typically given a clean bill of health. However, this overlooks a far more sensitive and earlier indicator of metabolic trouble: high fasting insulin. Insulin resistance is a condition where your cells become less responsive to the effects of insulin. To compensate and keep blood sugar levels normal, your pancreas is forced to work overtime, pumping out progressively more insulin. This compensatory phase can last for years, or even decades.
During this entire period, your fasting glucose may look perfectly normal, masking the intense underlying struggle. High circulating levels of insulin (hyperinsulinemia) are directly damaging to the arterial wall. Insulin is a growth hormone, and in excess, it promotes the proliferation of smooth muscle cells within the arterial walls. This process is a key component in the development of atherosclerotic plaques and directly contributes to the thickening and stiffening of the arteries. A high fasting insulin level is therefore a direct red flag for ongoing vascular damage, even with normal blood sugar.
The illustration below shows a conceptual cross-section of an artery, demonstrating how the wall thickens over time due to this smooth muscle cell proliferation driven by insulin resistance.
Requesting a fasting insulin test from your doctor provides a much clearer picture of your true metabolic health. It can reveal a problem long before it shows up as high blood sugar, offering a critical window of opportunity to intervene with diet and lifestyle changes to reverse the process before significant arterial damage is done. It is one of the most important, yet commonly overlooked, markers for premature vascular aging.
Why Does Slow Jogging Build More Energy Factories in Your Cells Than Sprinting?
The key to building cellular energy and improving vascular health lies in understanding two distinct types of exercise. High-intensity interval training (HIIT), or sprinting, is excellent for improving performance and glucose tolerance. However, when the goal is to fundamentally increase your body’s energy production capacity, long-duration, low-intensity exercise like slow jogging—often called “Zone 2” cardio—is superior. This is because it is the most potent stimulus for a process called mitochondrial biogenesis.
Mitochondria are the “energy factories” inside your cells. They are responsible for producing ATP, the fuel that powers everything you do. A greater number and efficiency of mitochondria mean your body is better at using fat for fuel, clearing lactate, and resisting fatigue. Zone 2 exercise specifically activates a signaling pathway known as PGC-1α, which is the master regulator of mitochondrial biogenesis. During these long, steady sessions, your body is under a sustained, low-level stress that signals it to build more mitochondria to meet the consistent energy demand.
Sprinting, by contrast, is an anaerobic activity that relies on different energy systems and does not stimulate the PGC-1α pathway as effectively for building this aerobic base. While HIIT has its place, an overemphasis on it without a strong aerobic foundation can lead to burnout and incomplete metabolic adaptations. Building a large base of mitochondria through Zone 2 training is fundamental for improving insulin sensitivity, reducing oxidative stress, and enhancing the overall health of your endothelial cells, which directly translates to more flexible arteries.
Your Action Plan: Optimal Exercise Protocol for Vascular Health
- Zone 2 cardio: Aim for 150+ minutes per week at a conversational pace, where you can speak in full sentences.
- Heart rate target: A general guideline is 180 minus your age to find your approximate Zone 2 heart rate ceiling.
- Session duration: Engage in sessions of at least 30-45 minutes to trigger the necessary mitochondrial adaptations.
- Frequency: Practice this 4-5 times per week to achieve and sustain improvements in arterial compliance.
- Complementary training: Add 1-2 HIIT sessions per week on top of your aerobic base for performance and metabolic flexibility benefits.
Key Takeaways
- Early arterial stiffness is primarily a disease of metabolic dysfunction, driven by factors like high blood sugar and insulin resistance, not just cholesterol.
- Specific nutrients, like the nitrates in beetroot juice and Vitamin K2, play a direct and active role in maintaining arterial flexibility and directing calcium properly.
- The type of exercise matters: low-intensity, long-duration cardio is superior for building the mitochondrial base necessary for long-term vascular health.
Why Is Cholesterol Not the Only Number That Matters for Your Heart?
For decades, the standard lipid panel—Total Cholesterol, LDL-C (“bad” cholesterol), and HDL-C (“good” cholesterol)—has been the cornerstone of cardiovascular risk assessment. While not irrelevant, an exclusive focus on these numbers provides an incomplete and sometimes misleading picture of your true risk. The critical insight that modern medicine has revealed is that the *number of atherogenic particles*, not just the total cholesterol they carry, is the primary driver of atherosclerosis.
Imagine two scenarios: in one, you have a few large, fluffy LDL particles carrying a certain amount of cholesterol. In the other, you have many small, dense LDL particles carrying the exact same amount of cholesterol. The second scenario is far more dangerous because the higher number of particles dramatically increases the probability that some will penetrate the arterial wall and initiate plaque formation. Advanced lipid testing provides a much more granular view by measuring particle numbers and other crucial markers.
This table compares the traditional markers you’re used to seeing with the more advanced markers that give a clearer assessment of vascular risk.
| Traditional Markers | Advanced Markers | What They Measure |
|---|---|---|
| Total Cholesterol | ApoB (Apolipoprotein B) | The total number of all potentially atherogenic particles (a much better risk indicator). |
| LDL-C | LDL-P (LDL Particle Number) | The actual count of LDL particles, which is more predictive than their cholesterol content. |
| HDL-C | hs-CRP (high-sensitivity C-Reactive Protein) | The level of systemic inflammation, a key driver of plaque rupture. |
| Triglycerides | Lp-PLA2 | An enzyme indicating vascular-specific inflammation within the artery wall itself. |
Furthermore, direct measures of arterial stiffness, like Pulse Wave Velocity (PWV), offer a real-world assessment of your vascular health that goes beyond blood markers. In fact, the Framingham Heart Study revealed that individuals in the lowest quartile of pulse wave velocity had a significantly lower incidence of adverse cardiovascular outcomes. Focusing only on cholesterol is like trying to understand traffic congestion by only counting the number of buses, ignoring the hundreds of cars, motorcycles, and trucks that are actually causing the jam. To truly understand and manage your risk, you must look beyond the traditional numbers.
Now that you understand the hidden drivers of arterial stiffness, the logical next step is to take proactive control. To effectively manage your vascular health, start a conversation with your healthcare provider about ordering advanced lipid panels (like ApoB and LDL-P) and a fasting insulin test. This data will provide a far more accurate picture of your risk and allow for a targeted strategy to ensure your arteries remain flexible and youthful for decades to come.